The 7 Stages of Dementia: What They Are and What To Expect

A dementia diagnosis is a progressive condition, meaning it gets worse over time. Symptoms of dementia include memory loss and reduced problem-solving, language, and motor skills. This loss of cognitive function results in a person’s inability to perform daily activities independently. While every individual is unique, their journey typically follows a specific progression. There are seven stages of dementia, and each progressive level comes with both new symptoms and a worsening of existing symptoms. Understanding the seven dementia stages and related symptoms will help you determine when it’s time to reassess your family member’s care needs.
Let our care assessment guide you
Our free tool provides options, advice, and next steps based on your unique situation.
Key Takeaways
- There are seven stages of dementia, each with distinct symptoms. The stages are broken down into three phases of pre-, middle-, and late-stage dementia.
- Dementia typically isn’t diagnosed until stage 4. Dementia stages 1, 2, and 3 are classified as pre-dementia stages, as symptoms aren’t yet severe enough for a diagnosis.
- There’s no set timeline for how long each stage will last. Understanding the symptoms associated with each stage will help you monitor your loved one as the disease progresses.
- Memory care communities can help. Explore how thoughtfully designed memory care communities can support your loved one at any stage.
What are the seven stages of dementia?
Health care providers use a comprehensive tool to assess the seven stages of dementia in the elderly called the Global Deterioration Scale.[01] Also known as the GDS, this trusted method enables caregivers and health professionals to determine how quickly dementia is progressing in an elderly patient. It also helps families and care providers know which symptoms to expect during each of the seven stages of dementia.
Learning about the dementia stages can help caregivers track and monitor stage-related symptoms to identify a loved one’s brain-health status.
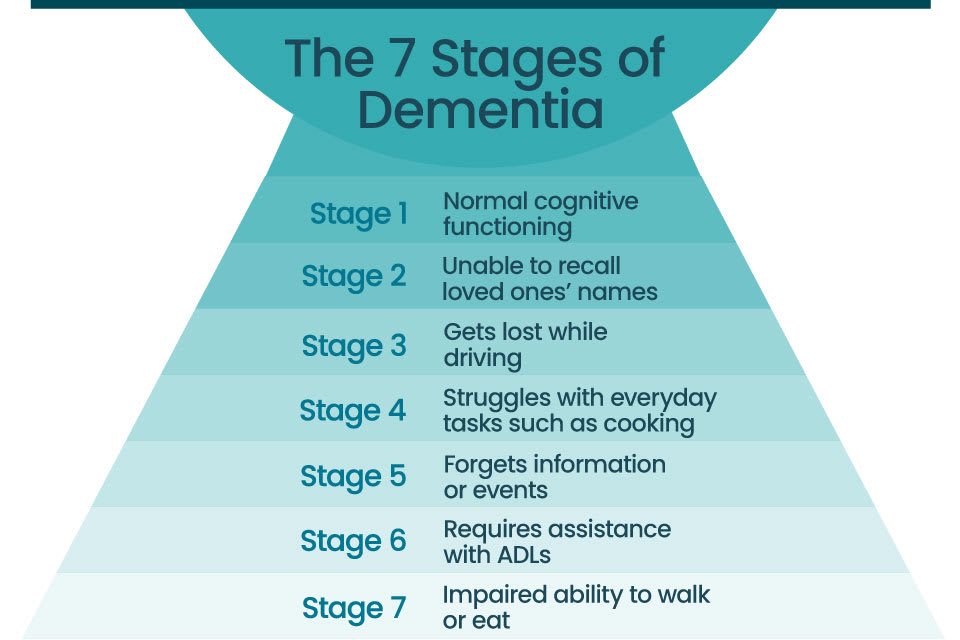
The seven stages of dementia include:
- Stage 1: no cognitive impairment
- Stage 2: very mild cognitive decline
- Stage 3: mild cognitive decline
- Stage 4: moderate cognitive decline
- Stage 5: moderately severe cognitive decline
- Stage 6: severe cognitive decline
- Stage 7: very severe cognitive decline
How does dementia progress?
The seven stages are separated into three progressive phases or levels of dementia:
- Pre-dementia or early-stage dementia (stages 1, 2, and 3). In this initial phase, a person can still live independently and may not exhibit obvious memory loss or have any difficulty completing regular tasks. Mild dementia symptoms mimic episodes of age-related forgetfulness.
- Moderate or middle-stage dementia (stages 4 and 5). Moderate dementia symptoms significantly affect a person’s personality and behavior. Someone with middle-stage dementia will generally need full- or part-time caregiver assistance with regular day-to-day activities. Moderate-stage dementia symptoms include significant cognitive impairment and mood swings.
- Severe or late-stage dementia (stages 6 and 7). These final phases are associated with severe cognitive impairment along with a loss of physical abilities. Late dementia symptoms can include pronounced memory loss, incontinence, and an inability to move without help.
Specific types of dementias — including Alzheimer’s, vascular, Lewy body, and frontotemporal dementia — advance at unique rates and differ from person to person. Therefore, it’s important to understand the signs and symptoms at each stage so you can quickly identify whether your loved one’s dementia has progressed. Read on for a look at the symptoms related to each stage.
Dementia stage 1: No cognitive impairment
Though it may sound odd, stage 1 dementia often looks like normal mental functioning without any cognitive decline. Someone in the first three stages of dementia doesn’t usually exhibit enough symptoms to be diagnosed.
While mild cognitive impairment may be present, stages 1, 2, and 3 on the GDS are recognized as pre-dementia stages. However, it’s important to note that changes in the brain are still taking place in these early stages, which could eventually lead to a dementia diagnosis at stage 4.

Let our care assessment guide you
Our free tool provides options, advice, and next steps based on your unique situation.
Dementia stage 2: Very mild cognitive decline
Stage 2 dementia includes simple memory mistakes like a loved one wondering, “Where did I put my keys?” or “What was that person’s name?” This is a pre-dementia stage and does not yet warrant an official dementia diagnosis.
A significant portion of the senior population experiences age-related forgetfulness, and caregivers or medical providers may not even notice such a mild impairment. This explains why stage 2 is also known as “age-associated memory impairment” on the GDS, meaning many older adults will experience symptoms like these at some point during aging.
“About 40% of people aged 65 or older have age-associated memory impairment — in the United States, about 16 million people,” said Professor Gary W. Small in research published by the British Medical Association.[02] “Only about 1% of them will progress to dementia each year.”
This means that for many people, pre-dementia stage 2 does not progress to an official dementia diagnosis. Seniors can maintain at this stage for a long time or indefinitely with the right lifestyle changes that support their brain health.
Stage 2 dementia symptoms include:
- Losing track of familiar objects
- Inability to recall names of friends, family members, and former acquaintances

Talk with a Senior Living Advisor
Our advisors help 300,000 families each year find the right senior care for their loved ones.
Dementia stage 3: Mild cognitive decline
Stage 3 dementia is also known as mild cognitive impairment (MCI) or decline. It doesn’t generally have a major effect on day-to-day functioning and may not yet result in an official dementia diagnosis. Memory and cognitive problems may become more regular and noticeable to caregivers and family members.
How quickly can this early dementia stage progress to a dementia diagnosis in the elderly?
An estimated 10 to 20 percent of people age 65 or older with MCI will develop recognizable or diagnosable dementia within a year, according to the National Institute on Aging.[03]
Since MCI can precede more severe dementia, it’s important to recognize these stage 3 signs, and seek medical advice to support your brain health and keep the dementia from progressing.
Stage 3 dementia symptoms include:
- Often forgetting to go to appointments or events
- Losing things often
- Getting lost while traveling
- Decreased work performance
- Difficulty finding the right words
- Verbal repetition
- Challenges with organization and concentration
- Trouble with complex tasks and problem-solving
- Problems with driving
Dementia stage 4: Moderate cognitive decline
Stage 4 dementia is when a person has clear, visible signs of cognitive impairment and also exhibits personality changes, with significant dementia behaviors and severe stage 3 symptoms. A person is not typically diagnosed with dementia until they’re at stage 4 or beyond.
While the medical terminology for stage 4 dementia is moderate cognitive decline, this stage is officially diagnosed by the GDS as “mild dementia.” At this stage, doctors and caregivers will likely observe hallmark signs that dementia is getting worse, including difficulties with language and reduced problem-solving skills.
Stage 4 dementia symptoms include:
- Social withdrawal
- Emotional moodiness
- Lack of responsiveness
- Reduced intellectual sharpness
- Trouble with routine tasks
- Forgetting recent events
- Denial of symptoms
Dementia stage 5: Moderately severe cognitive decline
This stage marks the onset of what many professionals refer to as middle-stage dementia or “mid-stage” in the seven stages of dementia. At this point, a person may no longer be able to carry out normal activities of daily living (ADLs), such as dressing or bathing, or instrumental activities of daily living (IADLs) without some caregiver assistance.
Stage 5 often lasts between two and four years, though every dementia patient will progress at a unique rate.[04]
In stage 5 dementia, your loved one will likely require more intense support and supervision. They know major facts about themselves — such as their name and their children’s names — but they may not remember their grandchildren’s names, their longtime address, or where they went to high school.
Stage 5 dementia symptoms include:
- Pronounced memory loss, including personal details and current events
- Wandering
- Confusion and forgetfulness
- Disorientation and sundown syndrome
- Further reduced mental acuity and problem-solving ability
Dementia stage 6: Severe cognitive decline
Stage 6 dementia marks a need for caregiver help to perform basic daily activities, such as eating, using the toilet, and other self-care. Seniors experiencing this stage of moderately severe dementia may have difficulty regulating sleep, interacting with others, or behaving appropriately in public settings.
At stage 6 of dementia, you may find yourself wondering if full-time care is necessary as symptoms become more complex. You can stay prepared by tracking symptoms, monitoring your loved one’s ability to perform activities of daily living (ADLs) and instrumental activities of daily living (IADLs), and exploring care options like memory care or home care.
Stage 6 dementia symptoms include:
- Sleep difficulties
- Urinary or fecal incontinence
- Aggression and anxiety
- Personality changes including paranoia or delusions
- Inability to perform activities of daily living (ADLs)
- Pronounced memory loss
- Inability to recognize loved ones and caregivers
Dementia stage 7: Very severe cognitive decline
In stage 7, which is considered end-stage dementia, people can no longer care for themselves and are barely responsive as their verbal and physical capacities shut down. All verbal ability is lost, movement becomes severely impaired, and bodily organs begin to fail.
Stage 7 dementia symptoms include:
- Inability to speak
- Inability to remember loved ones or caregivers
- Lack of physical ability to move without help
- Inability to chew or swallow
- Impaired bodily functions, including breathing, and organ failure
- Sleeping a lot
- Urinary and fecal incontinence
How long does this aggressive end stage of dementia last?
The final stage of dementia can typically last one to three years, but it’s difficult to predict since everyone is different.[05]
How fast does dementia progress?
There’s no way to predict how long it will take for a loved one to progress through all the stages of dementia. Lifestyle factors can make a big difference in how fast dementia will progress, like diet and exercise.
Dementia gets worse with time, but some people stay in the early stages of dementia longer and can remain independent for many years. Others may experience rapid dementia progression and will require more immediate support. Once a person reaches the final, most aggressive stage of dementia, they typically only have a couple years left.[05]
How long do people live with dementia?
The average person with a dementia diagnosis can live between four to eight years after diagnosis.[05] Some people, however, can live up to 20 years after their diagnosis.
Different types of dementias, like Alzheimer’s disease and vascular dementia, have different prognoses, with some causing more rapid deterioration than others. Individual factors like lifestyle and treatment plans are critical in slowing down the progression of dementia.
Here’s a general outline of the average life expectancies across different dementias, according to the Alzheimer’s Society:[06]
- Alzheimer’s disease. The life expectancy range is between eight and 10 years.
- Vascular dementia. People with vascular dementia face additional risk factors like stroke or heart attack, and the average life span is five years.
- Lewy body dementia. A greater threat of injuries and infections places the life expectancy for dementia with Lewy bodies at around six years.
- Frontotemporal dementia. The expected lifespan ranges from six to eight years.
How to care for a loved one with dementia
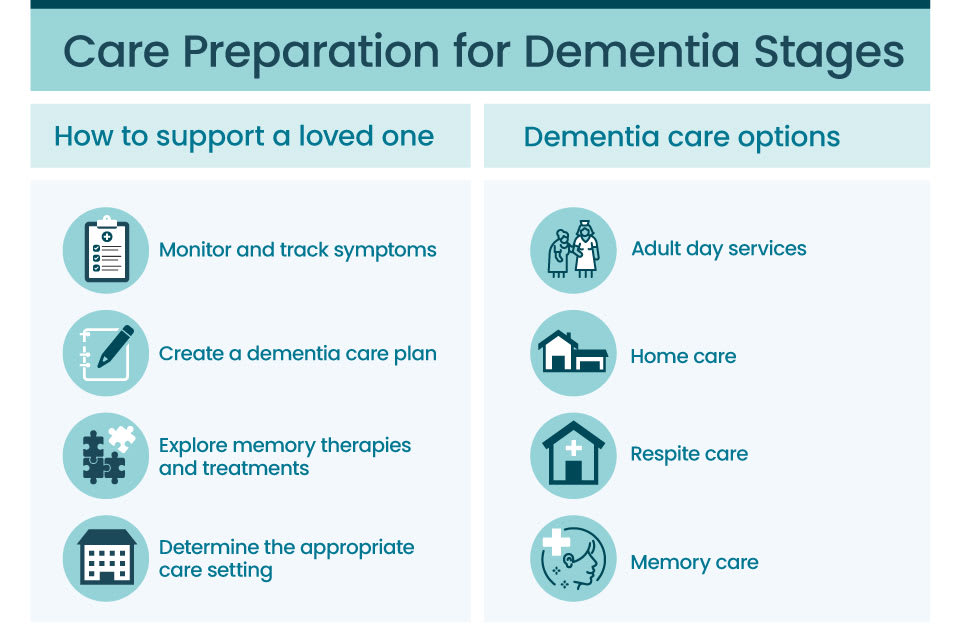
Caregivers have a variety of ways to provide support to a loved one through the progression of dementia:
- Try to have positive and meaningful conversations using effective dementia communication strategies.
- Consider exploring unique dementia treatment options and therapies.
- Create a dementia care plan.
- Consider joining a support group for caregivers.
- Learn about dementia care techniques for caregivers.
- Find memory care options in your area.
Coming to accept a loved one’s dementia diagnosis, and understanding what to expect, can help you feel empowered and provide opportunities to make the most of this time together.
If the idea of navigating a dementia diagnosis alone seems overwhelming, A Place for Mom is here for you. Explore our library of caregiver resources, which contains hundreds of articles covering dementia therapies and information on memory care communities.
Memory care options
Memory care is specialized support for seniors with a dementia diagnosis. These communities provide 24-hour supervision by trained memory care caregivers to reduce anxiety, assist with ADLs, and prevent accidents caused by wandering.
Memory care communities also provide comfortable and thoughtfully designed living arrangements, meal services, and trained on-site nurses ready administer health care as needed. Therapeutic on-site memory care activities, dining plans, and exercise programs (for both mind and body) address all types of dementia symptoms. Whether through in-home care or at a community, specialized memory care can be beneficial from the early stages of dementia through the end of life.
Understanding when to seek memory care will vary depending on a senior’s dementia symptoms, health status, living situation, and more. Our Senior Living Advisors offer free guidance and are ready to discuss local memory care communities or dementia home care options with your family, tailored to your budget and individualized needs.
Key Takeaways
Reisberg, B. Ferris, S. de Leon, M., & Crook, T. (1982). The global deterioration scale for assessment of primary degenerative dementia. American Journal of Psychiatry.
Small, G. (2002, June 22). What we need to know about age related memory loss. The BMJ.
National Institute on Aging. National Institutes of Health. (2021, April 12). What is mild cognitive impairment?
Alzheimer’s Society. (2021, February 24). The middle stage of dementia.
Alzheimer’s Society. (2021, June 18). The later stage of dementia.
Alzheimer’s Association. Stages of Alzheimer’s.
Senior living options in all states
The information contained on this page is for informational purposes only and is not intended to constitute medical, legal or financial advice or create a professional relationship between A Place for Mom and the reader. Always seek the advice of your health care provider, attorney or financial advisor with respect to any particular matter, and do not act or refrain from acting on the basis of anything you have read on this site. Links to third-party websites are only for the convenience of the reader; A Place for Mom does not endorse the contents of the third-party sites.
Make the best senior care decision
Make the best senior care decision