
End-Stage Dementia: What to Expect and How to Offer Care

As seniors advance into end-stage dementia, their care needs will likely require full-time support, whether at home or in a care facility. The final stages of dementia — also called late-stage and advanced dementia — severely affect a person’s memory, communication, and ability to perform daily activities.
As a caregiver, you’ll likely face new physical and mental challenges as your loved one moves into the last stages of dementia. Recognizing end-stage dementia signs early will help you better anticipate when extra support is necessary.
Let our care assessment guide you
Our free tool provides options, advice, and next steps based on your unique situation.
Key Takeaways
- End-stage dementia usually requires full-time care. A person can lose their ability to communicate and require complete assistance with daily tasks.
- There's an increased risk of health concerns. Someone at this stage of the disease is usually in a frail condition with a weak immune system, which makes them more likely to develop other illnesses and medical problems.
- End-of-life care, such as palliative or hospice care, can help provide comfort during the final stages of dementia. Staff can help monitor loved ones and relieve pain.
- Advance care planning is necessary early on. It's important to establish medical decisions and final wishes before a loved one reaches end-stage dementia.
What are the signs of end-stage dementia?
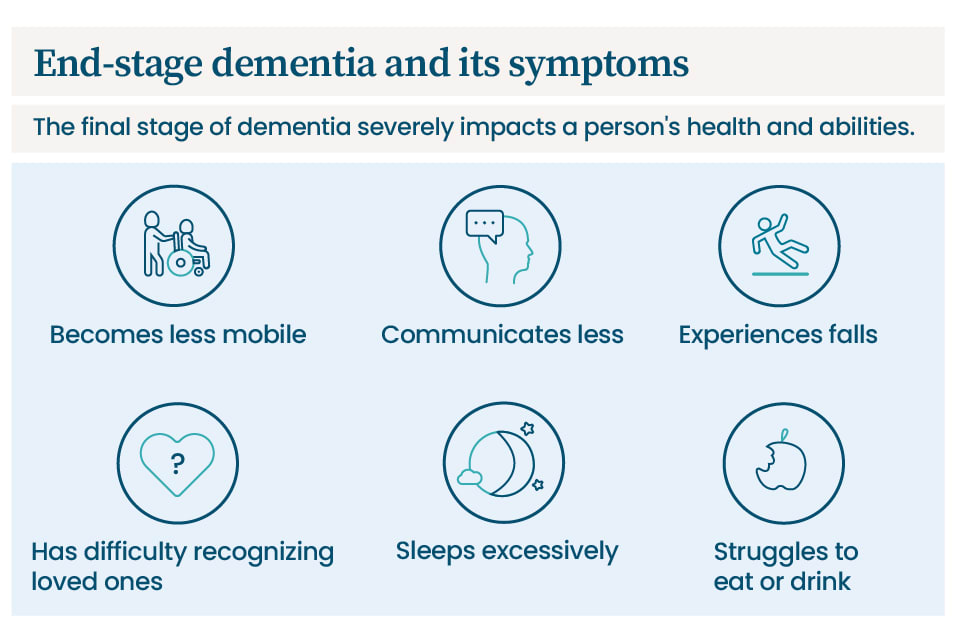
During end-stage dementia, a person loses their ability to communicate and experiences a decline in their physical capabilities, often requiring total assistance with daily tasks. Although a person can have end-stage dementia symptoms that indicate they’re nearing the end of life, they can continue living with those symptoms for several months or even years.[01]
These include:
- Sleeping all the time
- Falling and getting infections more often
- Having trouble recognizing family and friends
- “Time-shifting,” or believing they’re in a different time period
- Having difficulty eating, drinking, and swallowing
- Becoming frailer and less mobile
- Speaking less often
End-stage dementia life expectancy
The life expectancy for those with end-stage dementia can range from one to three years,[02] depending on factors such as:
- Gender
- Age at time of diagnosis
- Disease progression and severity
- Presence of other serious illnesses
The type of dementia a person has can also influence how fast the dementia progresses and how long end-stage dementia lasts. This stage is often shorter than prior phases of dementia because, at this point, a person is frail and has a weakened immune response. This makes them more susceptible to medical problems like pneumonia or blood clots.

Let our care assessment guide you
Our free tool provides options, advice, and next steps based on your unique situation.
End-of-life signs in dementia patients
Some symptoms of late-stage dementia may indicate the person is at the final stage of their condition. It’s important to recognize symptoms of the later stages of dementia before death to make sure your loved one receives the right amount of care at that time.
It’s difficult to pinpoint exactly when this time is given the variability of dementia progression, but a person may be nearing the end of their life if they have most, or all, of the following symptoms:
- Needing help with most daily activities
- Eating less and choking on food or liquids
- Limiting speech to single words or phrases that don’t make sense
- Being unable to walk or stand, or having trouble sitting up or getting out of bed without assistance
- Experiencing bladder and bowel incontinence
- Showing limited understanding of what’s said to them
Late-stage care options
The one-on-one care needs of a person with end-stage dementia may be too demanding for a family caregiver to take on alone. There are several resources available to provide support to caregivers throughout the later stages of the disease.
Palliative care
Palliative care provides comfort care and pain relief for anybody with a serious illness. Unlike hospice care, it’s available regardless of how long someone is expected to live, and a person doesn’t have to give up treatment for a serious illness.
Palliative care primarily focuses on improving quality of life and managing symptoms. It doesn’t replace medical care and can include the following additional services:
- Nutritional guidance and support
- Mitigation of pain or discomfort with medication
- Discussion of what to expect about the end of life with the patient and family
- Holistic support of the patient and their loved ones
Palliative care can be provided in a variety of settings, including:
- Hospitals
- Outpatient palliative clinics
- Patients’ homes
- Nursing homes
A person can begin receiving palliative care at the time of the dementia diagnosis. If the ongoing treatment doesn’t seem to be working anymore, the palliative care team can continue providing comfort care or transition into hospice care.
Hospice care

Hospice is end-of-life care for patients with a serious illness and a life expectancy of six months or less. It’s provided by a team of doctors, nurses, and other trained volunteers, and it offers the following up to 24 hours a day:
- Respite care
- Pain management
- Medical supplies and equipment
- Prescription drugs (for symptom relief, not disease treatment)
- Bereavement counseling
- Spiritual support
- Psychological and social services
Like palliative care, hospice care can take place in whatever setting the patient is most comfortable in, which can include:
- A patient’s home
- Hospice facilities
- Hospitals
- Nursing homes
- Assisted living facilities
Questions to ask about end-of-life care
An estimated 1.8 million people in the United States are in the final stages of dementia and will eventually require end-of-life care.[03] When weighing the different medical options available for end-of-life care, it’s important to understand how a palliative or hospice care team will meet the needs of the person with late-stage dementia.
You can determine this by asking the palliative or hospice care team specific questions about their approach to end-of-life care for someone with advanced dementia, such as:
- Does your team offer both palliative and hospice care?
- Is the team available to provide round-the-clock care?
- What specialized services are available to improve the patient’s comfort?
- Where can you provide care for someone with advanced dementia?
- Does the team have experience working with people living with dementia?
- How do your approaches to care affect a patient’s quality of life?

Talk with a Senior Living Advisor
Our advisors help 300,000 families each year find the right senior care for their loved ones.
The importance of planning ahead
A person in the final stages of dementia may not be capable of making decisions for long-term and end-of-life care, so advanced planning is essential to fulfilling their last wishes. While it can be difficult to have conversations about the end, advance care planning can make sure your loved one has the right support throughout the last stages of dementia.
Dementia progression is different for everyone living with the disease, so it’s important to have conversations early on and gather documents to establish medical decisions and estate plan wishes. Some possible documents include:
- Do-not-resuscitate order (DNR), which instructs medical providers to not perform CPR if a patient’s breathing stops or if their heart stops beating
- Living will, which provides specific instructions for end-of-life medical care
- Durable power of attorney for health care, which gives a designated person the power to make decisions about the patient’s medical care
- Will, which states how a person’s assets and estate should be distributed after death
- Living trust, which gives a designated trustee the authority to manage and distribute an individual’s assets after they pass
- Durable power of attorney for finances, which designates a person to make legal and financial decisions on behalf of the patient
Please consult an estate planning or elder law attorney for more information about these documents and the legal requirements involved.
The final stages of dementia can be overwhelming and exhausting for a caregiver, but they don’t have to be endured alone. A Place for Mom’s Senior Living Advisors are ready to learn about your loved one’s care needs and discuss available care options near you.
Social Care Institute for Excellence. (2020, March). Care in the last days of life with dementia.
Samaritan Healthcare & Hospice. End-stage dementia: What is it and when is hospice called in?
Zvi Aminoff, B. & Adunsky, A. (2006, August 22). Their last 6 months: Suffering and survival of end-stage dementia patients. Age and Ageing.
Senior living options in all states
The information contained on this page is for informational purposes only and is not intended to constitute medical, legal or financial advice or create a professional relationship between A Place for Mom and the reader. Always seek the advice of your health care provider, attorney or financial advisor with respect to any particular matter, and do not act or refrain from acting on the basis of anything you have read on this site. Links to third-party websites are only for the convenience of the reader; A Place for Mom does not endorse the contents of the third-party sites.
Make the best senior care decision
Make the best senior care decision